Psoriasis Articles
Biologic Vs Conventional Therapies: Comparing Risk of Psoriasis-Associated Comorbidities
Psoriasis is associated with multiple comorbidities. In this retrospective cohort analysis, we compared the comorbidities in patients who received biologic treatments with those who received conventio…
Cross-Sectional Study of Psoriasis, Atopic Dermatitis, Rosacea, and Alopecia Areata Suggests Association With Cardiovascular Diseases
Background: A growing body of evidence suggests that several inflammatory skin diseases (ISDs) are associated with systemic inflammation and cardiovascular disease (CVDs). Methods: We used the TriNet…
Evaluating Sentiment, Engagement, and Perception of Biologics Among Patients
With Psoriasis and Psoriatic Arthritis on Reddit
Background: Limited analyses of social media content among psoriasis (PsO) and psoriatic arthritis (PsA) patients exist. These patients may turn to social media to gain insight into treatments such as biologics.
Patient Preference for Calcipotriene and Betamethasone Dipropionate Cream
Versus Foam for the Topical Treatment of Psoriasis: A Pilot Study
Background: The well-established sequential use of topical calcipotriene and topical betamethasone dipropionate in combination has been shown to provide greater benefit than either monotherapy. A newer topical fixed combination formulation of calcipotriene 0.005% and betamethasone dipropionate 0.064% in a cream base (Cal/BD cream) is effective with high patient ratings for convenience and tolerability. The current study compares patient satisfaction between Cal/BD foam and Cal/BD cream formulations.
Breaking the Frustrating Cycle of Topical Steroids in Psoriasis: A Review of a Novel Vehicle for Fixed-Dose Combination Halobetasol Propionate/Tazarotene
Topical therapies are commonly used to treat psoriasis, either as monotherapy for milder disease or as adjuncts to systemic and biologic drugs. Topical steroids and tazarotene are both options for topical psoriasis treatment, but as monotherapies, they are associated with adverse events (AEs) that make adherence to prescribed treatment challenging.
Meeting Patient Expectations of Topical Psoriasis Treatment: Evidence Supporting the Use of Fixed-Combination Halobetasol/Tazarotene Lotion
Discordance between patient and clinician treatment goals and expectations can present a challenge to implementation of effective therapeutic plans…
Efficacy and Safety of Water-Free Lipid Formulation System Containing Calcipotriol Against Psoriasis Vulgaris
Calcipotriol, a vitamin D analogue is widely used in the treatment of psoriasis. However, poor adherence to topical therapy has led to an ineffective use of the medication and built a barrier to the treatment’s success…
An Investigator-Initiated Trial of a Polymeric Emulsion of Halobetasol Propionate and Tazarotene in the Treatment of Palmoplantar Psoriasis
Objective: To evaluate the synergistic effect of a fixed-combination topical lotion composed of halobetasol propionate 0.01% and tazarotene 0.045% in the treatment of palmoplantar psoriasis.
Examining the Potential for Koebnerization and Disease Precipitation in Cicatricial Alopecias
The treatment of primary scarring alopecias is challenging and patients may be susceptible to koebnerization. This predisposes cicatricial alopecia patients to worsening of their disease following procedural treatments or interventions.
Biological Therapy Interruption and Re-Treatment in Chronic Plaque Psoriasis
While biological treatments for chronic plaque psoriasis should be administered continuously to maximize and maintain efficacy, interruptions in therapy may be necessary for a number of reasons. We reviewed the evidence from clinical trials on efficacy, safety and immunogenicity in clinical trials for approved biologic agents for chronic plaque psoriasis. A systematic search of three major medical databases was performed and a total of 35 articles were included into the analysis, including 13 controlled trials. J Drugs Dermatol. 2021;20(10):1063-1071. doi:10.36849/JDD.5716 Read more.
A Retrospective Review of Patients’ Response to Biologic Therapy for Psoriasis
Jerry Bagel MD MS, Brianna Butler MS PA-C, Elise Nelson LPN CCRC, Alexa Hetzel MS PA-C
Biologic treatments have taken the forefront in treating moderate-to-severe psoriasis. Although numerous randomized, controlled trials have demonstrated the efficacy of these agents, there is limited data suggesting that clinical trial outcomes are reproducible in real-world patients. J Drugs Dermatol. 20(4):442-449. doi:10.36849/JDD.2021.5823 Read more.
Sponsored
Assessing the Risk of PDE4 Use for Psoriasis During the COVID-19 Pandemic
Donovan G. Kearns, Shelley Uppal PhD, Vipawee S. Chat, Jashin J. Wu MD
As the COVID-19 pandemic persists globally, physicians continue to assess the safety and benefit of immunomodulatory medications, in order to reduce the risk of infection or worsened disease outcomes in patients. While there is emerging evidence that targeted immunosuppression may be helpful in cases of severe COVID-19 infection with cytokine storm, this effect cannot be generalized to all immunomodulatory medications. J Drugs Dermatol. 2021;20(05):582
Once-Daily Novel Lotion for Moderate-to-Severe Plaque Psoriasis: Phase 3 Analysis of Hispanic Participants
Seemal R. Desai MD, Brad Glick DO MPH, James Q. Del Rosso DO, Susan Harris MS, Abby Jacobson MS PA-C
Psoriasis is a chronic, inflammatory disease that may differ in prevalence and clinical presentation among patients from various racial and ethnic groups. Two phase 3 studies demonstrated efficacy and safety of a novel 0.01% lotion in the treatment of moderate-to-severe plaque psoriasis (NCT02514577, NCT02515097). These post hoc analyses evaluated HP 0.01% lotion in Hispanic participants. J Drugs Dermatol. 20(3):252-258. doi:10.36849/JDD.2021.5698
Stay up-to-date on new clinical findings in Psoriasis.View the latest articles, case reports, supplements, podcast episodes and more!
Home | Articles | Case Reports | Supplements | Podcast Episodes | Translational Videos
Podcast Episodes
What Women Don’t Want … Psoriasis
Picking up on Prescribing Patterns for Psoriasis: A Real Deal Assessment
We are fortunate to live during a time when we have many safe and effective options to treat a chronic inflammatory skin disease such as Psoriasis. How does clinical trial efficacy and long term use translate to the real world and practical issues such as access, patient and practitioner perception? In a JDD Podcast, two investigators share their work and first steps to evaluate.
To Treat or Not To Treat: Systemic Therapy Considerations for Psoriasis in the Setting of Malignancy
In most phase 3 studies patients are weeded out or the history of malignancy must be at least 5 years prior to entry. So what to do? Our colleagues at Tufts Medical Center asked this very question. Tune in to hear what Dr. David Rosmarin learned from performing a retrospective chart review and how his work and his experience guides his clinical decision making when managing psoriasis.
Ask the Investigator: Shedding Some Light on Phototherapy Protocols for Psoriasis and Tips to Improve Patient Screening and Treatment
Dr. Adam Friedman reviews phototherapy protocols and pearls with psoriasis expert Dr. Jashin Wu. Also tune in to hear how Dr. Wu counsels his psoriasis patients on psoriasis comorbidities and initiates, and manages them with phototherapy, topicals, and systemic immunosuppressants.
Translational Lecture Series
Targeting cAMP Signaling for the Treatment of Inflammatory Diseases of the Skin
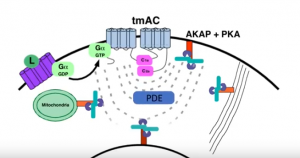 Dr. Jon Zippin elucidates the complexity of cAMP biology and the translational impact of PDE4 inhibition as it relates to chronic inflammatory skin diseases. Tune in to learn why targeting this pathway is clinically meaningful but also where more work is needed to improve outcomes.
Dr. Jon Zippin elucidates the complexity of cAMP biology and the translational impact of PDE4 inhibition as it relates to chronic inflammatory skin diseases. Tune in to learn why targeting this pathway is clinically meaningful but also where more work is needed to improve outcomes.
Psoriasis: Biological Basis for Comorbidities
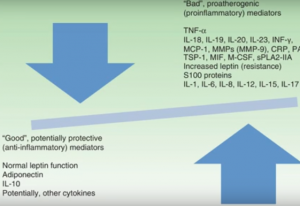 Dr. Abrar Qureshi, Professor and Chair of Department of Dermatology at The Warren Alpert Medical School of Brown University, reviews his research to uncover the biological basis for many of the co-morbidities associated with, and risk factors for, psoriasis. Through this clear and clinically oriented presentation, the common pathophysiological threads are elucidated with a focus on identifying preventive strategies and therapeutic targets for current and future treatments.
Dr. Abrar Qureshi, Professor and Chair of Department of Dermatology at The Warren Alpert Medical School of Brown University, reviews his research to uncover the biological basis for many of the co-morbidities associated with, and risk factors for, psoriasis. Through this clear and clinically oriented presentation, the common pathophysiological threads are elucidated with a focus on identifying preventive strategies and therapeutic targets for current and future treatments.






