the patient upon learning of the diagnosis of skin cancer and
the need for Mohs surgery. Furthermore, contributing factors
such as discussion of the biopsy result with the physician or
staff, discussion about what to expect on the day of surgery,
and determination if patients reviewed any informational materials
about the procedure were surveyed.
Within one week following Mohs surgery, a follow-up survey
was conducted to determine patients’ level of anxiety upon
arrival at the surgical appointment, their overall satisfaction
regarding the experience, and information regarding detailed
events and experiences that occurred during the surgical process
such as number of layers taken and activities performed
while the patient waited for each layer to be processed.
Survey data was compiled using the REDCap program and analyzed
with Microsoft Excel.
Limitations
This study was conducted at a single institution using the patients
of two Mohs surgeons. Expanding the patient base to
include a multi-center study would generate a larger sample
size as well as control for confounding variables. Also, surveys
were conducted at various time points within one week before
and after the surgery date. Standardizing the timing in which
surveys are conducted will minimize the significance of recall
bias. The surveys were also conducted orally by an interviewer
who knew the patient’s name, potentially reducing the patient’s
perception of anonymity. Therefore, it is a possibility that patients
felt compelled to report an inflated satisfaction score or
otherwise answer as they believed the interviewer would want
them to answer.
RESULTS
36 patients completed the survey. Of those sampled, the mean
age was 66 years, 18 were male, and 18 were female. All were
Caucasian, and two identified themselves as Hispanic or Latino.
15 (42%) reported having Mohs surgery before while 21 (58%)
had not.
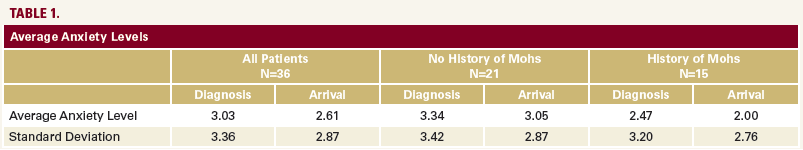
On a scale from 0 to 10, in which 0 represents “no anxietyâ€
and 10 represents “severe anxietyâ€, the respondents’ average
anxiety levels at the time of diagnosis and upon arrival for the
surgery day are reported in Table 1.
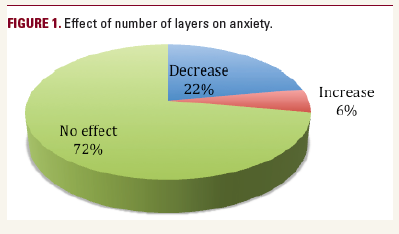
20% of the surveyed patients had an increased level of anxiety
upon arrival for surgery compared to the time of their diagnosis.
47% had no change in anxiety between diagnosis and
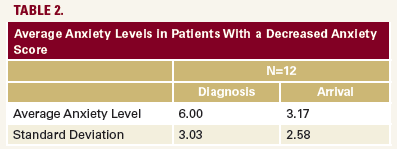
the surgery day. 12 of 36 patients (33%) had a decreased level
of anxiety upon arrival for surgery compared to the time of
their diagnosis. These 12 patients reported average anxiety of
6.0 (SD 3.03) at the time of diagnosis and 3.17 (SD 2.58) upon
arrival for surgery (Table 2). Of those 12, 9 (75%) reported at
least one factor that may have contributed to the decrease in
anxiety including a call discussing the biopsy result and skin
cancer diagnosis, a call discussing the Mohs procedure and
what to expect on the surgery day, reviewing written material
explaining Mohs surgery, and reviewing information regarding
Mohs surgery on the internet.
Of all the patients surveyed, approximately 20% reported a
subjective decrease in anxiety prior to the day of surgery by
receiving a call from a doctor or a nurse to discuss the skin
cancer diagnosis.
Of all patients who were called by a doctor, 26% reported subjectively
decreased anxiety while only 14% called by a nurse
reported subjectively decreased anxiety.