Stay up-to-date on new clinical findings and images in Atopic Dermatitis.
Atopic Dermatitis
Articles
Increased Risk of Subcutaneous Nodules and Lipomas Following Influenza Vaccination: A Multicenter TriNetX Cohort Study
Influenza vaccination represents one of the most widespread public health interventions. Localized cutaneous reactions, including nodules and pruritus, may occur rarely following vaccination, particularly when administered improperly. Our clinic observations suggest the potential development of lipomas following intramuscular vaccination.
Keeping Cool: An Updated Review on Cold-Induced Dermatoses and Cold-Associated Injury
The skin’s protective role as the first defense against environmental exposures makes it susceptible to climatic stressors.
Effects on the Skin Microbiome by a Moisturizer Formulated for Eczema-Prone and Sensitive Skin
Cutaneous dysbiosis contributes to the pathophysiology of atopic dermatitis and potentially that of sensitive skin; regulation of the bacterial communities through skincare products is an emerging management strategy.
Dupilumab Treatment Improves Lichenification in Atopic Dermatitis in Different Age and Racial Groups
Lichenification, common in moderate to severe atopic dermatitis (AD) at any age, is often difficult to treat. This analysis assessed dupilumab vs placebo in AD lichenification by age and race-defined groups.
A Brief Report of Thirteen Cases of Poppers Dermatitis
Poppers are psychoactive inhalants commonly employed in the gay male community for their ability to relax anal sphincter muscles.1 These drugs induce numerous adverse effects including dizziness, retinal degeneration, headache, maculopathies, fatal methemoglobinemia, and contact dermatitis.2,3
Topical Treatment of Atopic Dermatitis: An Adherence-Based Appraisal of the AAD Guidelines
Atopic dermatitis (AD) places a financial and illness burden on children and adults and is the most common chronic inflammatory skin disease.
Assessing Patient Preferences for Atopic Dermatitis Treatment: A Review Article of Discrete Choice Experiments
Atopic dermatitis (AD) is one of the most prevalent inflammatory skin conditions, characterized by recurrent eczema with varying degrees of erythema, pruritus, xerosis, and pain. Although there are many treatment options for AD, efficacy is limited by poor adherence, especially for topical medications.
A Consensus on Staphylococcus Aureus Exacerbated Atopic Dermatitis and the Need for a Novel Treatment
The skin microbiome is essential for skin barrier function because it inhibits pathogen colonization, and decreased microbiome diversity correlates with increased Staphylococcus aureus (S. aureus) burden and atopic dermatitis (AD) severity.
Safety and Tolerance Evaluation of a Suncare Product in Ethnically Diverse Children With Atopic Dermatitis-Prone Skin
Atopic Dermatitis (AD) is a common chronic inflammatory skin condition, with high prevalence in children. Sun protection is important for children with eczema and AD-prone skin, yet many sunscreens can cause skin irritation due to their formulations. In this study, we evaluated the safety and tolerance of an SPF 50 sunscreen in ethnically diverse children with a history of AD over 4 weeks of product use.
Image Analysis of Xerosis and Atopic Dermatitis Following Prebiotic Skincare Regimen in Ethnically Diverse Patients
Variations in the epidemiology, clinical presentation, and disease course in atopic dermatitis (AD) patients with Skin of Color (SOC) compared with white counterparts have been reported. In this study, we evaluated the capability of a new imaging device (SkinCam) in quantifying skin texture changes in diverse patients, presenting with AD or xerosis, after using a prebiotic skincare routine over 10 weeks.
Analysis of Reddit Reveals JAK Inhibitor Questions Among Atopic Dermatitis Patients
Reddit is a popular social media website that is increasingly being used as a source of health information and discussion, especially among the younger population. We analyzed the subreddit “eczeJAKs” (a group whose “about” statement is: “Janus Kinase Inhibitors for Th2 Dermatitis”), and found many gaps in patient knowledge, showing areas for future improvement.
Attenuation of Atopic Dermatitis in Newborns, Infants, and Children With Prescription Treatment and Ceramide-Containing Skin Care: A Systematic Literature Review and Consensus
Atopic dermatitis (AD) typically starts in infancy and early childhood. The chronic skin disorder is associated with recurrent flares, pruritus, and genetic predisposition.
Efficacy of a Prebiotic Skincare Regimen on Improving Mild Atopic Dermatitis and Severe Xerosis in Diverse Ethnically Patients
Atopic Dermatitis (AD) is a chronic relapsing inflammatory skin disease associated with a significant patient burden on quality-of-life.
Recent Advances in Skincare Management of Atopic Dermatitis in Diverse Racial and Ethnic Groups
Atopic Dermatitis (AD) is a chronic relapsing inflammatory skin disease associated with a significant patient burden on quality-of-life.
Real-World Patient Cases Using Botanical Serum-Containing Corrective Gel as an Adjunct to Aesthetic Facial Laser or Microneedling Radiofrequency (MRF) Treatment
Integrated skin care is defined as the complementary use of topical treatments to nonsurgical facial rejuvenation procedures, such as lasers and radiofrequency microneedling devices…
Selection of Nemolizumab Clinical Dosage for Atopic Dermatitis
Nemolizumab is a monoclonal antibody directed against the interleukin-31 receptor A subunit, which is involved in the pathogenesis of pruritus and inflammation in atopic dermatitis (AD)…
Ant Venom-Based Ceramide Therapy Is Effective Against Atopic Dermatitis In Vivo
Background: Atopic dermatitis (AD) is a common skin condition with relatively few therapeutic alternatives. These include corticosteroids, which address inflammation but not superinfection, and Januse kinase (JAK) inhibitors, which have a US Food and Drug Administration (FDA) black box for potential carcinogenicity.
Cross-Sectional Study of Psoriasis, Atopic Dermatitis, Rosacea, and Alopecia Areata Suggests Association With Cardiovascular Diseases
Background: A growing body of evidence suggests that several inflammatory skin diseases (ISDs) are associated with systemic inflammation and cardiovascular disease (CVDs).
Sequential Treatment With Topical Trifarotene and Injectable NASHA Gel in Acne Scars: A Case Series
Background: Topical retinoids are a mainstay in acne management and have been shown to improve skin texture. Injectable non-animal stabilized hyaluronic acid (NASHATM) gel as skin booster is largely used in aesthetic treatments to improve skin quality including the appearance of atrophic acne scars.
A Qualitative Study on Product's Impact on Atopic Dermatitis Among Adolescent and Adult Patients
Objective: To qualitatively assess the life experiences and impact of treatment in adult and adolescent patients with AD being treated with this product.
The Safety and Efficacy of Roflumilast Cream 0.15% and 0.05% in Patients With Atopic Dermatitis: Randomized, Double-Blind, Phase 2 Proof of Concept Study
Background: Patients with atopic dermatitis (AD) need safe and effective topical treatments.
Objective: To assess safety and efficacy of a specific cream in patients with mild to moderate AD.
Analysis of Reddit Reveals Dupilumab Questions Among Atopic Dermatitis Patients
Atopic dermatitis patients are turning to social media to seek guidance and source medical information. Reddit, the seventh most visited website in the US, contains the popular “eczeMABs” subreddit, a forum dedicated to discussing monoclonal antibody therapy for atopic dermatitis.
Patient Questions about Atopic Dermatitis from Reddit
Atopic dermatitis and eczema patient questions remain unanswered as they turn to Reddit. Reddit, the seventh most visited website in the US with approximately 430 million monthly active users, has become a popular platform for patients to source medical information and discuss diseases. See their questions, frustrations and insights.
The Heterogeneity of Atopic Dermatitis
Atopic dermatitis (AD) is a chronic and burdensome inflammatory skin disease. This narrow and overly simplified description overlooks the heterogeneity of AD. While itch is the most prevalent and burdensome symptom of AD,skin-pain is one of several other symptoms that contribute to disease-burden.
Topical S. aureus – Targeting Endolysin Significantly Improves Symptoms and QoL in Individuals With Atopic Dermatitis
Atopic dermatitis (AD) is a chronic skin condition affecting an increasing number of children and adults whose quality of life is impacted by chronic itch and pain. It is characterized by an altered epidermal barrier, skin inflammation, and skin microbiome dysbiosis particularly over-colonization of Staphylococcus aureus.
Case Reports
Pustular Psoriasis Appearing Induced by Therapy in a Patient With Atopic Dermatitis
A treatment inhibits T-helper 2 (Th2)-driven inflammation cascade by blocking interleukin-4 (IL-4) and IL-13 signaling, which has been recognized to play a crucial role in the pathogenesis of atopic dermatitis (AD) and shown encouraging efficacy on moderate to severe AD.1 We report an interesting Chinese AD case, which developed into pustular psoriasis after treatment.
Treatment for Prurigo Nodularis and Pruritis
Prurigo nodularis (PN) is a disease in which chronic scratching and picking of the skin due to intense pruritis results in papulonodules, notably in areas that are accessible to the patient. The pathophysiology is hypothesized to be mediated by a Th2 helper cell response, similar to that seen in atopic dermatitis, therefore, treatment of PN would be expected to elicit a therapeutic response.
Translational Lecture Series
Targeting cAMP Signaling for the Treatment of Inflammatory Diseases of the Skin
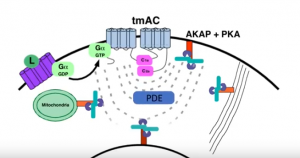 Dr. Jon Zippin, Assistant Attending Dermatologist and Assistant Professor of Dermatology at Weill Medical College of Cornell, elucidates the complexity of cAMP biology and the translational impact of PDE4 inhibition as it relates to chronic inflammatory skin diseases. Tune in to learn why targeting this pathway is clinically meaningful but also where more work is needed to improve outcomes.
Dr. Jon Zippin, Assistant Attending Dermatologist and Assistant Professor of Dermatology at Weill Medical College of Cornell, elucidates the complexity of cAMP biology and the translational impact of PDE4 inhibition as it relates to chronic inflammatory skin diseases. Tune in to learn why targeting this pathway is clinically meaningful but also where more work is needed to improve outcomes.
Update on Pediatric Inflammatory Skin Disorders: How Pathogenesis Informs Treatment
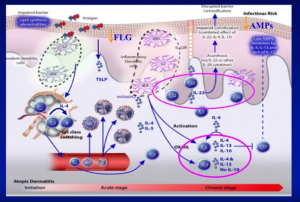 Dr. Amy Paller, Walter J. Hamlin Professor and Chair of Dermatology & Professor of Pediatrics at Northwestern University Feinberg School of Medicine in Chicago, Illinois, delivers a presentation discussing the cause and treatment of pediatric Atopic Dematitis, including co-morbidities, epidermal barrier impairment, and compliance issues.
Dr. Amy Paller, Walter J. Hamlin Professor and Chair of Dermatology & Professor of Pediatrics at Northwestern University Feinberg School of Medicine in Chicago, Illinois, delivers a presentation discussing the cause and treatment of pediatric Atopic Dematitis, including co-morbidities, epidermal barrier impairment, and compliance issues.
Itch form Bedside to Bench
 Dr. Gil Yosipovitch, Professor of Dermatology at University of Miami Miller School of Medicine, provides residents and physicians access to the latest bench research and practical pearls from a master in pruritus that will help them offer the highest quality evidence-based dermatological care.
Dr. Gil Yosipovitch, Professor of Dermatology at University of Miami Miller School of Medicine, provides residents and physicians access to the latest bench research and practical pearls from a master in pruritus that will help them offer the highest quality evidence-based dermatological care.
Advertisement
Podcast Episodes
Atopic Dermatitis (AD) is the second most common chronic inflammatory (coming for you acne!) which unapologetically imparts a tremendous burden on society as a whole. But what if you could jump in the DeLorean with Doc Brown, rev up to 88 miles per hour, and go back in time to stop it in the first place…would you?
Special Considerations for Managing Eczema in the Elderly
Atopic dermatitis does not discriminate. The second most common inflammatory skin disease (coming for you, acne vulgaris) can be appreciated across all demographics which contributes to the insane heterogeneity about which we are commonly taught. Unique considerations and approaches must be employed to ensure a personalized approach. Join Dr. Katrina Abuabara, Associate Professor of Epidemiology and Dermatology at UCSF, as she reviews her approach to caring for the geriatric AD population and their caregivers with JDD Podcast host Dr. Adam Friedman. This topic never gets old!
This podcast series is supported by Pfizer.
Don’t Fear, Getting Involved with NEA is Oh So Clear
Cutting the cord for residency training can feel like losing one’s Netflix account, distanced from the epicenter of cultural or dermatologic life. How to stay engaged, involved, or even keep your finger on the rapid pulse of innovation or development you ask? It’s as simple as sending an email. JDD Podcast host Dr. Adam Friedman takes a deep dive with National Eczema Association (NEA) Vice President of Scientific and Clinical Affairs Wendy Smith-Begolka on all paths to engagement. Education, research, community advocacy…it’s all there and a 5 gm sample tube throw away (meaning real close). Tune in to learn how to continue the cutaneous connection.
This podcast series is supported by Pfizer.
Atopic Dermatitis Treatment – The Future Landscape
Hall of famers Dr.s Amy Paller and Jonathan Silverberg join host Dr. Adam Friedman to review current moderate to severe AD treatment approaches and use of systemic therapies, discuss advancement on AD clinical management with use of novel target therapy, and share clinical experience with the use of biologics treatment. As we have all been thrown a curve ball in life, faculty address the growing concerns surrounding dermatology-related immunosuppressant therapy during the pandemic and how to discuss this issue with patients. Slide into home with a peak at the future therapies landscape in clinical development.
Insights On the Pediatric, Adolescent & Adult AD Patient
Dr. Adam Friedman is joined by Dr. Lindsey Finklea, a practicing dermatologist and parent/caregiver of a child with severe atopic dermatitis, and Dr. Peter Lio, podcast veteran and AD focused Derm extraordinaire, to discuss the issues affecting patient-family/patient-caregiver interactions and offer clinical pearls for effective management strategies to best assist the needs of parents, families and caregivers for patients with the AD.
From Cutaneous Microbiota to Clinical Trial Recruitment… Diversity Matters
Unless you have been under a pile of retention hyperkeratosis, it would be hard to say one has not heard the call to purposefully diversify clinical trial programs to ensure data generated is truly generalizable, let alone better appreciate demographic based nuances of disease presentation. Now how much is that happening in the OTC space you ask? Well Dr. Zoe Draelos, former AAD V.P. and Clinical Trial G.O.A.T., will answer. Press play to pick apart how clinical studies evaluating over the counter products should be structured and rewind/listen twice for good luck to how to purposefully recruit a diverse group of subjects and tools to make it a reality. Best practices for picking clinically relevant and meaningful outcomes – check. Can a study evaluating a cleanser and moisturizer reveal new learnings and consideration? You betcha.
This podcast is funded by La Roche-Posay.
Perspectives on Managing Moderate-to-Severe Atopic Dermatitis
Join host Dr. Adam Friedman in this Atopic Dermatitis dedicated series as he parties with and picks the brains of dermatology powerhouses Dr.s April Armstrong and Lawrence Eichenfield on pursuing a practical and powerful process to partner with patients of all ages and partake in a long standing management strategy.
Current Understanding of the Pathophysiology, Etiology, Prevalence & Burden of AD
Dr. Adam Friedman is joined by the dynamic dermatitis duo Dr. Anna De Benedetto, Associate Professor of Dermatology at the University of Florida, and Dr. Eric Simpson, Professor of Dermatology at the School of Medicine at Oregon Health & Science University, to dissect established and emerging pathophysiologic details of this dastardly dermatitis.
Special Considerations for Managing Eczema in the Elderly
Atopic dermatitis does not discriminate. The second most common inflammatory skin disease (coming for you, acne vulgaris) can be appreciated across all demographics which contributes to the insane heterogeneity about which we are commonly taught. Unique considerations and approaches must be employed to ensure a personalized approach. Join Dr. Katrina Abuabara, Associate Professor of Epidemiology and Dermatology at UCSF, as she reviews her approach to caring for the geriatric AD population and their caregivers with JDD Podcast host Dr. Adam Friedman. This topic never gets old!
This podcast series is supported by Pfizer.
Don’t Fear, Getting Involved with NEA is Oh So Clear
Cutting the cord for residency training can feel like losing one’s Netflix account, distanced from the epicenter of cultural or dermatologic life. How to stay engaged, involved, or even keep your finger on the rapid pulse of innovation or development you ask? It’s as simple as sending an email. JDD Podcast host Dr. Adam Friedman takes a deep dive with National Eczema Association (NEA) Vice President of Scientific and Clinical Affairs Wendy Smith-Begolka on all paths to engagement. Education, research, community advocacy…it’s all there and a 5 gm sample tube throw away (meaning real close). Tune in to learn how to continue the cutaneous connection.
This podcast series is supported by Pfizer.
Atopic Dermatitis Treatment – The Future Landscape
Hall of famers Dr.s Amy Paller and Jonathan Silverberg join host Dr. Adam Friedman to review current moderate to severe AD treatment approaches and use of systemic therapies, discuss advancement on AD clinical management with use of novel target therapy, and share clinical experience with the use of biologics treatment. As we have all been thrown a curve ball in life, faculty address the growing concerns surrounding dermatology-related immunosuppressant therapy during the pandemic and how to discuss this issue with patients. Slide into home with a peak at the future therapies landscape in clinical development.
Reface the Chase: Paradigm shifts in the AD Management Strategy Mentality
Who doesn’t love a good game of “Whack a Mole?” Anyone? Just as you try to stay ahead of those furry, taunting, smiling devils that keep popping up as you try to get a score that doesn’t undercut your prowess in front of your children (speaking on behalf of a friend), the agita and stress from chasing AD flares can interfere with long term treatment adherence, success, and partnership between patient and derm.
Video Pearls
Breaking New Ground in Atopic Dermatitis Treatment: Dr. Linda Stein Gold Discusses the “Level Up” Study
At the recent Revolutionizing Atopic Dermatitis (RAD) conference, Dr. Linda Stein Gold, Director of Dermatology Clinical Research and Division Head of Dermatology at Henry Ford Health, presented pivotal data from the “Level Up” study—a head-to-head comparison of two advanced treatments for atopic dermatitis: Rinvoq and Dupixent. This study, conducted by AbbVie, sheds new light on therapeutic options for managing this challenging condition.
Supplements
Real-World Patient Cases Using Botanical Serum-Containing Corrective Gel as an Adjunct to Aesthetic Facial Energy-Based Device Treatments
Prebiotic Skincare Management of Atopic Dermatitis & Xerosis in Diverse Ethnically Patients
Atopic Dermatitis (AD) is a chronic relapsing inflammatory skin disease associated with a significant patient burden on quality-of-life. Rising evidence demonstrate skin microbiome playing an essential role in AD pathogenesis. A decrease in skin microbial diversity, particularly an overabundance of Staphylococcus aureus colonization, is observed on AD lesional skin, plus is associated with disease severity.
Management of Atopic Dermatitis
The treatment horizon for pediatric AD is encouraging. Newer pharmaceuticals are now joined by novel formulations of established medications, which arms dermatologists with an increasing array of treatments to tackle this challenging condition.
Next Steps in Derm
Sleep Like a Baby: Integrative Tips for Sleep in Atopic Dermatitis
Sleep is essential for our overall well-being and one of the pillars of atopic dermatitis management. Unfortunately, we don’t learn or talk about this much in dermatology. Don’t fret- Dr. Vivian Shi shares her integrative strategies for optimizing sleep in atopic dermatitis!
Controversies in Pediatric Dermatology: Systemic Therapies
Dr. Yasmine Kirkorian, Interim Chief of Dermatology at Children’s National Health System and Assistant Professor of Dermatology and Pediatrics at the George Washington School of Medicine & Health Sciences, summarizes recent controversies in the field of pediatric dermatology regarding the usage of systemic therapies in children.






