INTRODUCTION
Lichen Planus (LP) is an auto-inflammatory idiopathic condition with unclear etiology, believed to be an auto-reactive response of T-cell-mediated damage after exposure to an inciting antigen. LP presents as pruritic, violaceous papules and plaques most commonly on the volar wrists, flexural surfaces, and trunk. Histologically, LP is characterized by a band-like lichenoid lymphocytic infiltrate with vacuolar destruction of the basal layer.1 LP has no FDA-approved treatments. Typical off-label treatments are topical and systemic steroids, anti-malarials, retinoids, antibiotics, immunosuppressants, phototherapy, and recently, apremilast and oral and topical Janus kinase inhibitors.1,2 We present the case of a 70-year-old female with a history of LP and lichen planopilaris who experienced complete resolution of LP after using tapinarof 1% topical cream.
Case Presentation
A 70-year-old female presented to the clinic with complaints of scalp pruritus and pruritic eruption on bilateral shins lasting several weeks. Her medical history was significant for acid reflux, for which she was taking famotidine.
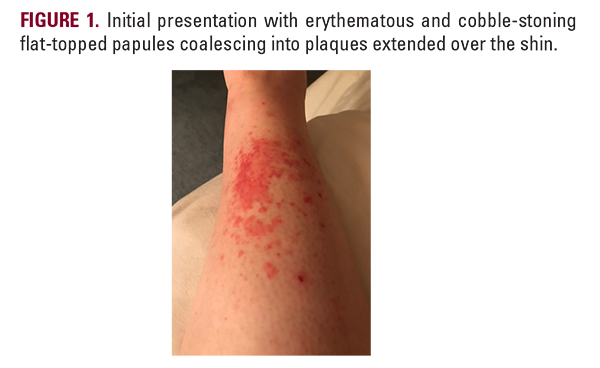
On examination, we observed erythema and subtle perifollicular scaling at the scalp, as well as erythematous and cobble-stoning flat-topped papules coalescing into plaques on the bilateral shins. She was treated for presumed seborrheic dermatitis with ketoconazole shampoo and clobetasol solution. Fluocinonide cream was prescribed for the shins.
Case Presentation
A 70-year-old female presented to the clinic with complaints of scalp pruritus and pruritic eruption on bilateral shins lasting several weeks. Her medical history was significant for acid reflux, for which she was taking famotidine.
On examination, we observed erythema and subtle perifollicular scaling at the scalp, as well as erythematous and cobble-stoning flat-topped papules coalescing into plaques on the bilateral shins. She was treated for presumed seborrheic dermatitis with ketoconazole shampoo and clobetasol solution. Fluocinonide cream was prescribed for the shins.
She returned after 2 months, reporting no improvement in either condition. Two biopsies were performed. The biopsy of the right temporal scalp showed hyperkeratosis of the epidermis and fibrosis with chronic inflammation centered around the hair follicles in the dermis. The biopsy of the right shin showed hyperkeratosis and hypergranulosis with a band-like lymphocytic infiltrate. These findings were consistent with lichen planopilaris and LP, respectively.
The patient was started on hydroxychloroquine 200 mg twice daily. Hepatitis C was negative. CBC and CMP were unremarkable. She denied mucus membrane or nail involvement. The scalp was treated with intralesional Kenalog 2.5 mg/mL. Pimecrolimus and compounded tofacitinib 2% creams were added.
The patient was started on hydroxychloroquine 200 mg twice daily. Hepatitis C was negative. CBC and CMP were unremarkable. She denied mucus membrane or nail involvement. The scalp was treated with intralesional Kenalog 2.5 mg/mL. Pimecrolimus and compounded tofacitinib 2% creams were added.






