To the Editor,
Chronic kidney disease (CKD) affects approximately 14% of adults nationally and is characterized by impaired immunity, systemic inflammation, and microvascular dysfunction.1,2 These physiologic disruptions impair wound healing and predispose patients to adverse surgical outcomes.1,2 Mohs micrographic surgery (MMS) is the gold standard for managing nonmelanoma skin cancer (NMSC), offering high cure rates while preserving healthy tissue.3 Given that MMS is frequently performed in medically complex patients,3 including those with CKD, understanding the postoperative risks in this population is critical. While CKD has been broadly linked to poor surgical outcomes,2 limited data exist on its impact on complication rates following MMS.
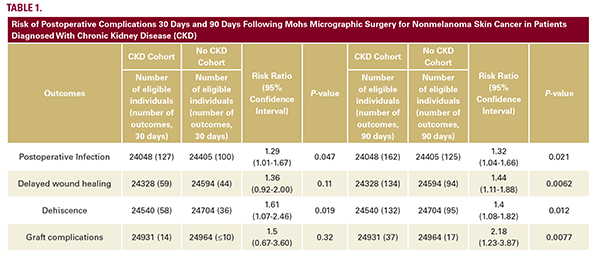
A retrospective cohort study was conducted using the TriNetX Research Network to evaluate the risk of postoperative complications in patients with CKD undergoing MMS for NMSC. Adults diagnosed with basal cell carcinoma (BCC) or squamous cell carcinoma (SCC) who underwent MMS between July 21, 2020, and July 21, 2025, were identified. Patients with CKD were identified using the International Classification of Diseases, 10th revision code (ICD-10-CM) for CKD (N18). Patients with inherited or acquired disorders that impair wound healing, systemic infection, or sepsis on the day of surgery, or documentation of previous postoperative complications were excluded. A comparator cohort of patients without CKD was generated using 1:1 propensity score matching on age, sex, race, ethnicity, immunosuppressant medication use, and relevant comorbidities, including obesity, smoking, diabetes mellitus, chronic venous insufficiency, and peripheral arterial disease. The final matched cohorts included 25,016 patients each. Postoperative outcomes were assessed at 30-days and 90- days after surgery with risk ratios (RR). Statistical significance was defined as a two-sided P-value <0.05.
Chronic kidney disease (CKD) affects approximately 14% of adults nationally and is characterized by impaired immunity, systemic inflammation, and microvascular dysfunction.1,2 These physiologic disruptions impair wound healing and predispose patients to adverse surgical outcomes.1,2 Mohs micrographic surgery (MMS) is the gold standard for managing nonmelanoma skin cancer (NMSC), offering high cure rates while preserving healthy tissue.3 Given that MMS is frequently performed in medically complex patients,3 including those with CKD, understanding the postoperative risks in this population is critical. While CKD has been broadly linked to poor surgical outcomes,2 limited data exist on its impact on complication rates following MMS.
A retrospective cohort study was conducted using the TriNetX Research Network to evaluate the risk of postoperative complications in patients with CKD undergoing MMS for NMSC. Adults diagnosed with basal cell carcinoma (BCC) or squamous cell carcinoma (SCC) who underwent MMS between July 21, 2020, and July 21, 2025, were identified. Patients with CKD were identified using the International Classification of Diseases, 10th revision code (ICD-10-CM) for CKD (N18). Patients with inherited or acquired disorders that impair wound healing, systemic infection, or sepsis on the day of surgery, or documentation of previous postoperative complications were excluded. A comparator cohort of patients without CKD was generated using 1:1 propensity score matching on age, sex, race, ethnicity, immunosuppressant medication use, and relevant comorbidities, including obesity, smoking, diabetes mellitus, chronic venous insufficiency, and peripheral arterial disease. The final matched cohorts included 25,016 patients each. Postoperative outcomes were assessed at 30-days and 90- days after surgery with risk ratios (RR). Statistical significance was defined as a two-sided P-value <0.05.