INTRODUCTION
Dissecting cellulitis of the scalp (DCS), also known as perifolliculitis capitis abscedens and suffodiens, is a form of neutrophilic cicatricial alopecia leading to irreversible hair loss.1 It presents with pustules, boggy fluctuant nodules and absecesses on the vertex and posterior scalp that evolve into sinuses and heal with scars. While its etiology remains unclear, follicular occlusion, together with bacteria-triggered aberrant immune response play an important role.1 Intralesional steroids, isotretinoin and oral antibiotics are the mainstay of treatment with often unsatisfactory results.1 We report a case of DCS recalcitrant to conventional treatment that responded to the IL17A inhibitor secukinumab.
CASE
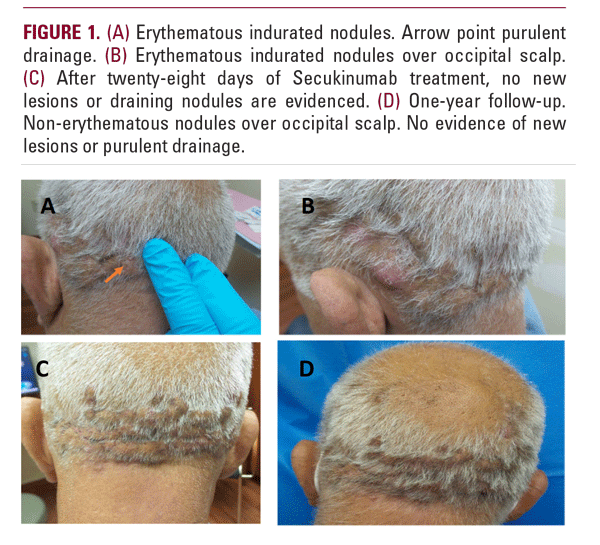
A 63-year-old male with history of acne vulgaris was referred to our clinic with a biopsy-confirmed diagnosis of dissecting cellulitis of his occipital scalp for more than four years. The patient had previously received multiple treatments including doxycycline, trimethoprim-sulfamethoxazole, clindamycin, rifampin, and adalimumab, which he was given for a three-month period. However, the disease progressed while on therapy. Finally, isotretinoin was prescribed precipitating a flare during the first month of use. On physical evaluation, the patient displayed scarring alopecia involving the occipital portion of the scalp with tender, fluctuant, purulent nodules (Figure 1A, 1B). The patient was started on oral dapsone 12.5 mg daily with gradual increase to 50 mg daily and concomitant intralesional triamcinolone 10 mg/cc. After three months, there was little symptomatic improvement, and the patient noted weekly flares. His physical exam was significant for new nodules with purulent secretion. Treatment with secukinumab 150 mg subcutaneous monthly injections after 4 weekly loading doses was initiated concomitantly with dapsone 50 mg daily. The patient injected 6 weekly doses in error and then continued for two more months of single injection each month. In total, the patient injected 8 injections of 150 mg over three months. The patient could not receive more medication due to lack of insurance coverage. Following one-month therapy, the patient’s drainage and pain completely stopped, and his nodules began regressing for the first time in six years (Figure 1C).
After the initiation of secukinumab, the patient developed an eczematous reaction for which he was treated topically. Other adverse events were not noted, and complete blood count values were stable. The patient remained in remission at one-year follow-up (Figure 1D).
After the initiation of secukinumab, the patient developed an eczematous reaction for which he was treated topically. Other adverse events were not noted, and complete blood count values were stable. The patient remained in remission at one-year follow-up (Figure 1D).

DISCUSSION
Data on treatment options of DCS is limited and no standard therapy exists. Several treatments have been utilized based on clinical severity with varying results including topical clindamycin, oral zinc, dapsone, isotretinoin, minocycline, sulfa drugs, quinolones, rifampin, metronidazole, glucocorticoids, tumor necrosis factor blockers, laser hair removal, ablative CO2 laser and surgical excision with and without grafting.1
Secukinumab is a human monoclonal anti–interleukin (IL)-17A antibody approved for the treatment of moderate to severe plaque psoriasis. It has been used off-label to treat other dermatological conditions including pityriasis rubra pilaris2-5 and HS.6-8 Given the clinical presentation and the recalcitrant nature of our patient’s pathology, we initiated secukinumab which binds with high selectivity to IL-17A, inhibiting the inflammatory cascade of activated neutrophils, lymphocytes
Secukinumab is a human monoclonal anti–interleukin (IL)-17A antibody approved for the treatment of moderate to severe plaque psoriasis. It has been used off-label to treat other dermatological conditions including pityriasis rubra pilaris2-5 and HS.6-8 Given the clinical presentation and the recalcitrant nature of our patient’s pathology, we initiated secukinumab which binds with high selectivity to IL-17A, inhibiting the inflammatory cascade of activated neutrophils, lymphocytes







