CASE REPORT
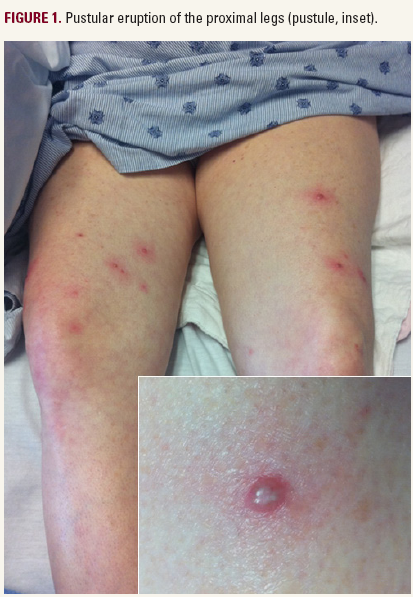
A 49-year-old woman presented with a four-day history of a pustular eruption on the face, chest and proximal extremities (Figures 1 and 2). The lesions were slightly
tender, but the patient was afebrile and otherwise well. Her medical history was significant for diabetes mellitus, dyslipidemia,
atrial fibrillation, stroke and treatment-resistant Graves disease. Her medications included lisinopril, metoprolol, phenytoin,
propylthiouracil, simvastatin and warfarin.
Two days prior to the onset of the eruption, she underwent a thyroid uptake scan with iodine-123. The next day she was administered iodine-131 for ablation of her thyroid. The pustular eruption began two days thereafter. A laboratory work-up revealed a normal hemogram; cultures of blood, pustules and lesional tissue were negative. A punch biopsy of a pustule revealed a dense dermal inflammatory infiltrate of neutrophils and intra epidermal neutrophilic micro abscesses
(Figure 3). With supportive care, all lesions resolved within six weeks.
DISCUSSION
Halogenoderma refers to skin eruptions caused by exposure to halides (iodide, bromide and fluoride). Iododerma is typically characterized by neutrophilic inflammatory infiltrates, manifest clinically as pustules. The eruption tends to favor regions where sebaceous glands are dense. If the mechanism of iodine exposure
is sudden and intense, an acute neutrophilic eruption may occur. In cases of more chronic low-grade exposure, the eruption
may be more insidious and the lesions assume a verrucous appearance. Chronic exposure to bromides (bromoderma) classically
leads to verrucous plaques with peripheral pustules.
Iododerma is a rarely reported complication of iodine ingestion. Cases of iododerma have occurred following administration of radioopaque iodinated contrast media1 and after topical application of iodine solutions.2 One report suggests that iododerma
may occur in up to two percent of patients who undergo radioiodide ablation of the thyroid.3 The pustular lesions of iododerma
resolve spontaneously as the iodide is cleared from the body. No specific treatment is necessary, but forced diuresis
may hasten resolution of the eruption.
DISCLOSURES
The authors have no relevant conflicts of interest to disclose






